Key Points:
- Patients with Alzheimer’s disease exhibit significantly lower levels of lithium in a brain region predominantly affected by Alzheimer’s disease, the prefrontal cortex.
- In aging people without Alzheimer’s disease, brain lithium levels correlate with cognitive test scores assessing how well individuals hold and manipulate information for problem-solving (known as working memory).
- Treatment with a low dose of a lithium salt restores memory in a mouse model of Alzheimer’s disease.
Researchers still do not have a comprehensive understanding of what causes the memory loss associated with Alzheimer’s disease. Pinpointing cellular factors, such as metal ion levels, which may, in part, cause memory loss in Alzheimer’s disease, could help unravel new ways to treat this devastating condition.
As published in Nature, Yankner and colleagues from Harvard University show that Alzheimer’s disease is associated with lower levels of lithium in the prefrontal cortex, a brain region adversely affected in patients with Alzheimer’s disease. Moreover, in aging people without Alzheimer’s disease, brain lithium levels were positively correlated with working memory. Furthermore, a lithium salt supplement (lithium orotate) restored memory in a mouse model of Alzheimer’s disease. These findings suggest lithium may serve as a treatment for Alzheimer’s disease, and more broadly, age-associated cognitive decline.
Lithium is a mood-stabilizing agent often prescribed to treat bipolar disorder. However, little research has linked lithium to age-related cognitive decline and specifically, cognitive decline associated with Alzheimer’s disease.
“The idea that lithium deficiency could be a cause of Alzheimer’s disease is new and suggests a different therapeutic approach,” said senior author of the study, Bruce Yankner, in a press release.
Alzheimer’s-Associated Brain Plaques Sequester Lithium
Lifestyle factors like diet or our environment can influence aspects of our physiology, like our metal ion levels. Previous research has focused primarily on the toxic effects of imbalances in levels of metals like iron, copper, and zinc and how these imbalances can influence Alzheimer’s-related plaque buildup in the brain. All the same, metals also have essential roles in brain function, and how altered levels of metals play a role in Alzheimer’s disease has remained unexplored.
To assess how balanced metal ion levels (known as metal-ion homeostasis) may play a role in Alzheimer’s disease, Yankner and colleagues assessed two brain regions. The two regions were the prefrontal cortex, a region highly affected by Alzheimer’s disease, and the cerebellum, a region mostly unaffected by Alzheimer’s disease. Yankner and colleagues made their assessments in cadavers from people with Alzheimer’s disease, with mild cognitive impairment (a precursor condition of Alzheimer’s disease), or without cognitive impairment.
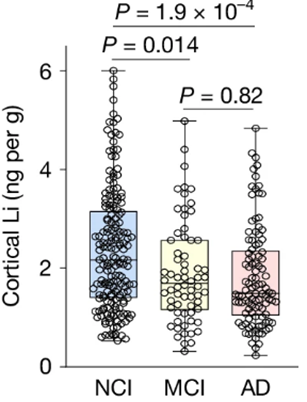
Interestingly, of the approximately 27 metal ions analyzed in the two brain regions, only lithium showed significantly reduced levels in the prefrontal cortex of individuals with either mild cognitive impairment or Alzheimer’s disease. These results suggest that lithium ion homeostasis in the brain becomes disrupted in people with mild cognitive impairment and Alzheimer’s disease.
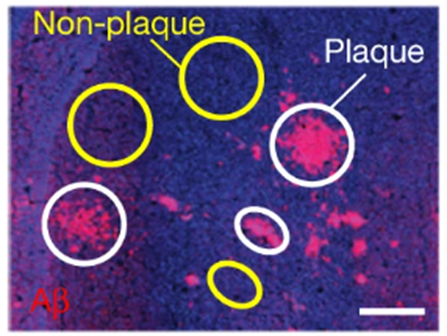
To investigate how lithium-ion homeostasis could be disrupted in patients with Alzheimer’s disease, the Harvard-based researchers turned to a mouse model for Alzheimer’s. With their mouse model, the Harvard-based researchers found that lithium concentrations were about three to four times higher in brain tissue with plaques. They also found that lithium levels in plaque-free brain tissue were significantly reduced in mice modeling Alzheimer’s compared to typical mice without Alzheimer’s pathology. These findings suggest that lithium somehow gets drawn into and sequestered by amyloid beta plaques.
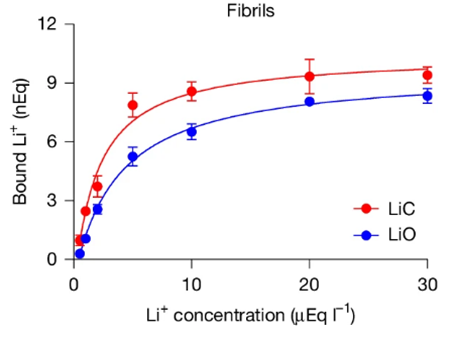
The data suggesting that amyloid beta plaques sequester lithium in Alzheimer’s disease prompted Yankner and colleagues to search for lithium salts, which are lithium ions bonded to a salt, that may not easily bind to the plaques. Of the lithium salts they analyzed, lithium orotate bonded to plaques at a significantly lesser degree in laboratory dishes than the standard lithium salt used clinically, lithium carbonate. These findings suggest that amyloid beta plaques may be less likely to sequester lithium orotate than lithium carbonate.
Lithium Orotate Treatment Reverses Memory Loss In Mice
Since amyloid beta plaques may not take up lithium orotate as easily as other forms of lithium, Yankner and colleagues decided to test whether administering lithium orotate to mice modeling Alzheimer’s could alleviate memory impairments. Interestingly, a low dose of lithium orotate treatment reversed memory loss in mice modeling Alzheimer’s disease, while lithium carbonate treatment did not. Moreover, a similar experiment was performed in naturally aged mice without Alzheimer’s disease, which showed that low-dose lithium orotate prevented an age-related decline in memory function. These findings suggest that less lithium orotate is sequestered by amyloid beta plaques, increasing lithium’s availability in the brain, which reverses memory deficits in Alzheimer’s disease. Furthermore, the results from naturally aged mice suggest that lithium orotate can preserve memory during natural aging.
Sufficient Lithium in the Brain Correlates with Memory Function
The findings suggesting that maintaining adequate lithium levels in the brain can preserve memory function prompted Yankner and colleagues to examine brain lithium levels and cognitive resilience in normal aging humans. The researchers found that brain lithium levels were positively correlated with scores on cognitive tests of memory capabilities related to holding and manipulating information for problem solving (known as working memory). These findings suggest that sufficient levels of lithium can help people preserve their working memory as they age.
Lithium Orotate Supplementation May Preserve Cognitive Resilience During Aging
Lithium is sometimes prescribed for the psychiatric condition bipolar disorder. The doses of lithium that patients with bipolar disorder are given, though, can be toxic to the kidneys when taken over extended periods. Along those lines, Yankner and colleagues used low doses of a lithium salt for their treatments, which conferred no toxicity with long-term administration to aging mice. As such, a low dose of daily lithium orotate may help preserve working memory as people age and may even serve as a key to memory restoration in mild cognitive impairment and Alzheimer’s disease without significant toxicity.
“One of the most galvanizing findings for us was that there were profound effects at this exquisitely low dose,” said Yankner.
Whether or not low-dose lithium orotate supplementation can confer memory-preserving effects during aging in humans and reverse memory loss in Alzheimer’s disease patients will require human trials for confirmation. Along those lines, some human trial data have already come out suggesting that daily low-dose lithium treatment over 15 months prevents loss of cognitive function in patients with Alzheimer’s disease. Moreover, sodium orotate supplements are available for purchase for anyone hedging their bet on the positive preclinical data in naturally aged mice and mice modeling Alzheimer’s disease.
“My hope is that lithium will do something more fundamental than anti-amyloid or anti-tau therapies, not just lessening but reversing cognitive decline and improving patients’ lives,” said Yankner.