Key Points:
- Heart attacks lead to scarring and damage that our heart cells cannot readily repair.
- Cellular reprogramming allows heart cells to divide in mice, which is necessary for heart repair.
- Following a heart attack in mice, cellular reprogramming repairs the heart and improves heart function.
The heart’s muscle cells, called cardiomyocytes (CM), must work in unison to deliver the force necessary for every beat. To produce each heartbeat, these heart cells rely on highly organized structures that generate mechanical force. However, scientists are finding that these structures must be dismantled before CMs can divide and regenerate the heart.
Now, researchers from the Chinese Academy of Medical Sciences report that cellular reprogramming can regenerate the heart. In the Journal of Molecular and Cellular Cardiology (JMCC), they show that cellular reprogramming stimulates CMs to divide fully. The findings fit with previous research suggesting that cellular reprogramming promotes health and longevity in animal models.
What Is Partial Cellular Reprogramming?
About 20 years ago, Japanese scientists made a major breakthrough: they showed that ordinary skin cells could be reprogrammed into stem cells. This Nobel Prize-winning feat depends on four genes, OSKM (Oct3/3, Sox2, Klf4, and c-Myc). Scientists have found that briefly activating these genes improves health and longevity in animals. This brief activation is known as partial cellular reprogramming.
More recently, researchers showed that this process can also work without c-Myc, a gene associated with cancer risk. Today, many scientists use the three-gene version, OSK, to study partial cellular reprogramming. When activated only briefly, OSK appears to make cells younger without fully turning them back into stem cells.
Cellular Reprogramming Induces Heart Cell Division
For CMs to proliferate and regenerate the heart, they must duplicate. To fully duplicate, they must divide. However, a key reason that adult hearts fail to meaningfully regenerate is that CMs do not readily divide. For this reason, the Chinese Academy of Medical Sciences researchers tested whether cellular reprogramming increases the division of CMs.
To induce cellular reprogramming, the researchers administered the OSK genes using gene therapy. The researchers also implemented a system that causes cells to fluoresce green or red when they fully divide. Remarkably, they found that the OSK gene therapy increased the number of single-colored cells, indicating the division of CMs.
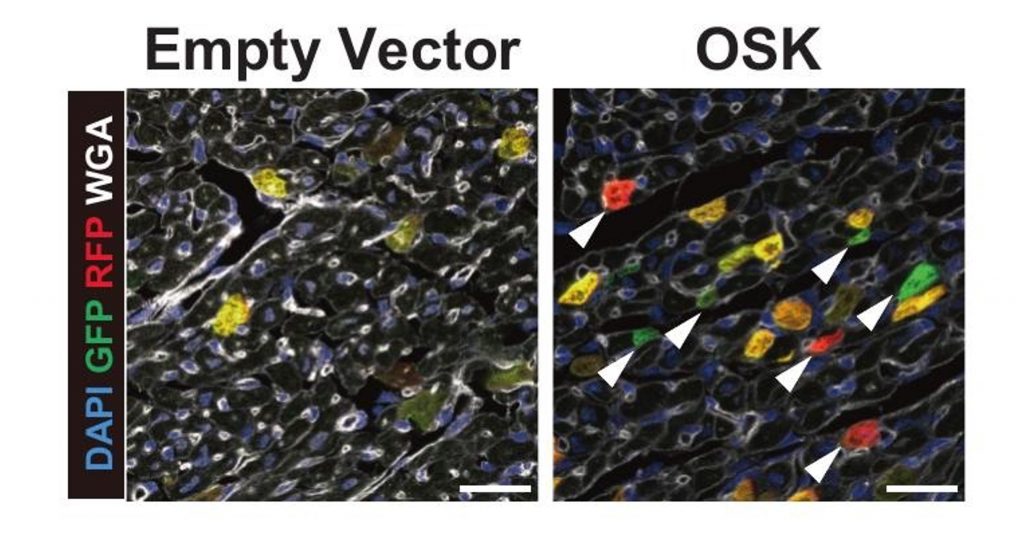
Dismantling Barriers
The barriers that keep CMs from dividing are called sarcomeres—highly ordered structures composed of protein filaments that generate force and allow the heart to pump blood. The researchers found that the OSK gene therapy dismantled the proteins associated with sarcomeres, suggesting that cellular reprogramming alleviates the structural barriers that make it difficult for CMs to divide.
Nevertheless, the heart’s ability to pump blood eventually deteriorated after about a month of therapy. The increase in sarcomere disassembly and cell division occurred when the mice were 14 days old (~9 human years), and there were no signs of heart defects. However, when the mice reached 28 days old (~12 human years), the researchers found that mice injected with the OSK genes showed signs of premature heart aging.
These findings demonstrate that cellular reprogramming improves the capacity of the heart to regenerate, but if activated for too long, the cellular reprogramming genes can damage the heart.
Cellular Reprogramming Improves Heart Regeneration Following Heart Attack
To test whether cellular reprogramming can regenerate the heart, the Chinese Academy researchers used a heart attack mouse model. During a heart attack, CMs lose oxygen and many die. In turn, the damaged area is usually replaced by scar tissue instead of new heart muscle tissue. However, if the CMs could divide and replace the dead CMs, they might be able to regenerate the heart muscle tissue and reduce scar tissue.
To trigger a heart attack in adult mice, the researchers temporarily blocked the coronary artery, which is the main artery supplying blood to the heart. Following the heart attack, the researchers administered the OSK gene therapy. Strikingly, while the blood-pumping function of the heart was diminished from the injury, it was improved by cellular reprogramming. Namely, the OSK gene therapy led to an increase in the volume of blood pumped by the most muscular chamber of the heart, the left ventricle.
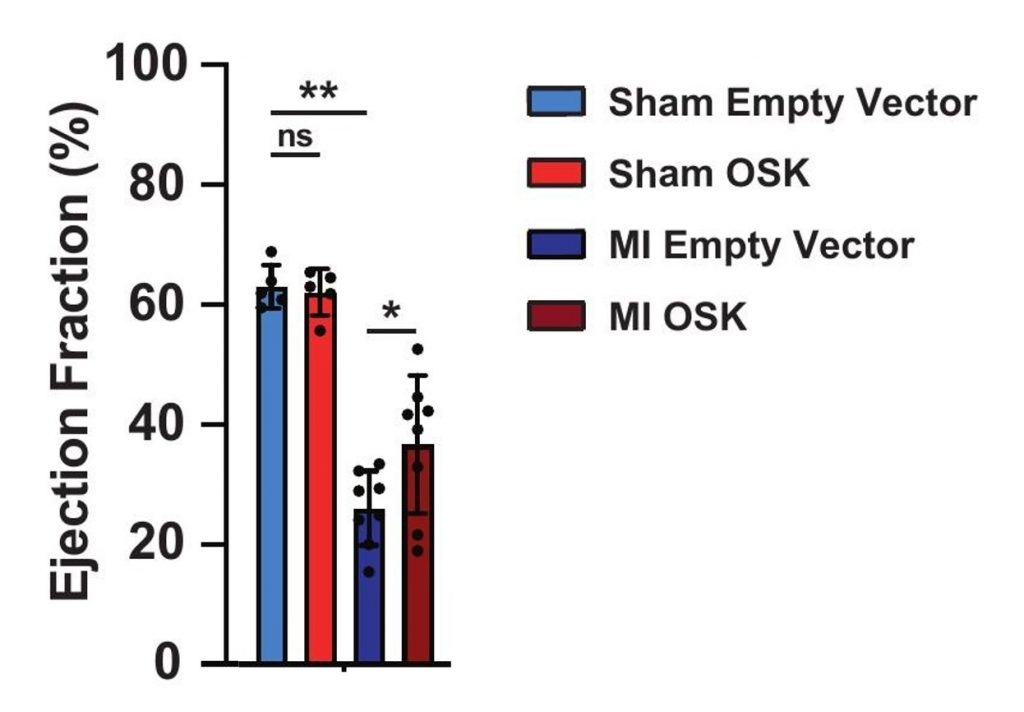
Crucially, the researchers found that the OSK gene therapy reduced heart scarring. The cellular reprogramming therapy also increased the number of proliferating cells near the site of damage, suggesting that the OSK gene therapy regenerates heart tissue. Based on these findings, the authors of the study conclude that cellular reprogramming promotes CM proliferation, heart muscle tissue regeneration, and functional recovery following a heart attack.
Testing Partial Cellular Reprogramming in Humans
According to Harvard Medical School, rising heart attack survival rates have increased the proportion of individuals with scarred and damaged hearts, contributing to an increase in heart failure. Heart attack survivors suffer from irregular heartbeats, fatigue, chest pain, reduced physical capacity, anxiety, and depression. It follows that regenerating the heart after a heart attack could lower the incidence of these adverse effects.
Whether cellular reprogramming gene therapy can alleviate heart attack-induced heart damage and scarring in humans remains to be tested. The FDA (Federal Drug Administration) recently approved the first human trial for testing partial cellular reprogramming gene therapy on the retina. If this trial is successful, it may open the door for testing partial cellular reprogramming gene therapy on heart attack survivors.